Vision: To improve the health of all the lives we touch.
Mission: To train Family Medicine physicians to provide high-quality, cost-effective care, to the greatest number of people possible in the region.

We are a group of clinicians and educators who strive to deliver outstanding care to patients within Gwinnett County and metro Atlanta while educating resident physicians to improve and promote the health care delivery system in the state of Georgia.
The principles of Family Medicine mandate healthcare that is comprehensive, continuous, and oriented toward the individual, their social support system, and the community.
The Family Physician is the point of entry for most patients requiring comprehensive health care. As the center of an interprofessional team of health care providers, we coordinate and advocate for the services of specialists and ancillary providers.
Our residents work with the hundreds of specialists within Gwinnett County, and our faculty train resident physicians in finding better ways to deliver cost-effective health services.
Our residents are exposed to all aspects of Family Medicine, providing them with the knowledge and skills to practice and deliver excellent health care.

We also have a strong focus on osteopathic training for residents who are interested in developing their osteopathic skills. This residency recognizes that personal maturity and self-awareness are an extremely important aspect of being a health care professional.
Upon graduation, our residents become physicians competent in providing comprehensive care to their patients, and have developed the skills required to be personally and professionally successful.
Northside Gwinnett Family Medicine Residency is an ACGME-accredited program and follows all rules and guidelines set forth by that governing body.
The Northside Hospital-Gwinnett Family Medicine Residency educates and trains resident physicians in the following locations:
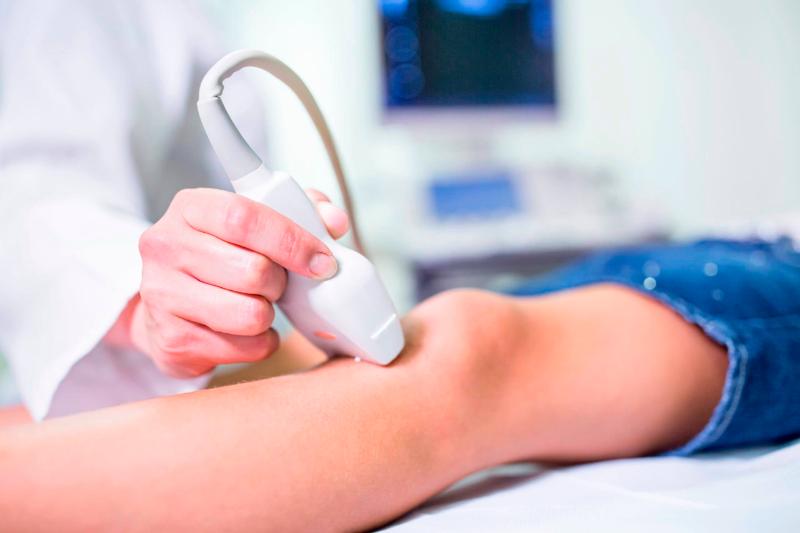
Strickland Family Medicine Center is the primary outpatient practice for the residency program. Residents have their continuity clinic and gynecology and dermatology procedure clinics here. Residents utilize point of care ultrasound within the clinical setting in identifying acute and chronic disorders.
Office procedures include circumcisions, gynecology procedures (endometrial biopsies, Long Acting Reversible Contraception insertions) and minor dermatology procedures (cryotherapy and skin biopsies).
Residents are able to provide continuity of care for the clinic patients in multiple settings, including in-patient and home visits.

Northside Hospital Duluth is the second hospital in our system. Inpatient, ICU, Night Float, emergency medicine, surgical-based rotations, and some electives take place at the Duluth location.

Northside Hospital Gwinnett is a tertiary care hospital located across the street from our family medicine practice. Obstetrics, emergency medicine, pediatric emergency medicine, newborn nursery, and some elective rotations take place at the Gwinnett location.
In addition, the Graduate Medical Education (GME) offices and classrooms are located in the lower level of Northside Gwinnett. The simulation lab, where residents experience immersive learning experiences allowing them to practice clinical procedures and gain expertise without risk of patient harm, is also located on this campus

Northside Hospital has an extensive network of high-quality specialty care. As such, residents have the opportunity to work with a wide range of specialty providers in their elective rotations.
Elective options include cardiology, nephrology, rheumatology, medical and surgical weight loss, ENT, wound care, endocrinology, and orthopedic surgery. Electives can also be tailored to a resident’s interest.

Mason Pediatrics is a pediatric practice located near Strickland Family Medicine Center. At Mason, residents gain experience in well-child exams, sports physicals, acute pediatric visits, and outpatient newborn care.



Our residents work with Sports Medicine fellows and faculty in Northside Orthopedic Institute in multiple settings ranging from the Concussion Institute to outpatient sports medicine clinics.
Our orthopedic specialists are team physicians for elite athletes at all levels of competition. Family medicine residents are invited to participate in sideline coverage for multiple athletic events.

Most of the geriatric experience is carried out at the Glancy Inpatient Rehabilitation Center, where residents work with PM&R physicians and ancillary staff to provide care to seniors and patients requiring post-hospital rehabilitation.
Additional geriatric experience is gained at Northside-Duluth and Strickland Family Medicine Center.
The Curriculum follows a four-week block schedule, allowing 13 blocks per academic year.
| PGY1 Year | # of weeks | PGY2 Year | # of weeks | PGY3 Year | # of weeks |
|---|---|---|---|---|---|
| Orientation | 4 | Behavioral Medicine | 4 | ||
| Systems-Based Practice | 4 | Surgery | 4 | ||
| Intensive Care | 2 | Sports Medicine | 4 | Sports Medicine | 4 |
| Emergency Medicine | 4 | Inpatient Pediatrics | 4 | Emergency Medicine | 4 |
| Outpatient Pediatrics | 4 | Electives | 8 | Electives | 20 |
| Newborn Nursery and NICU | 4 | Geriatrics | 4 | ||
| Pediatric Emergency Medicine | 4 | Pediatric Emergency Medicine | 4 | ||
| Inpatient Medicine | 12 | Inpatient Medicine | 8 | Inpatient Medicine | 4 |
| Maternity Care | 8 | Procedures | 4 | Procedures | 4 |
| Ambulatory Family Medicine | 6 | Ambulatory Family Medicine | 4 | Ambulatory Family Medicine | 8 |
| Night Float | 4 | Night Float | 4 | Night Float | 4 |
Wednesday Conference - Residents attend Family Medicine Grand Rounds and receive instructional education every Wednesday afternoon. The scope of conferences includes obstetrics, gynecology, adult medicine subspecialty and primary care, pediatrics, surgery, behavioral medicine, osteopathic manipulative therapy (OMT), and interprofessional education. In order to prepare them for independent practice, residents also complete training in cultural competency, practice management, diversity and inclusion, and physician self-care.
Safety Conference - Residents conduct a monthly interdisciplinary morbidity and mortality conference during which they have open discussions and analysis of recent cases. As a team, the residents and faculty collaborate to identify and address root causes of errors in order to improve quality of care and inform future practice.
The program received Osteopathic recognition from the ACGME and AOA in 2017.
The Osteopathic residents are instructed in and practice Osteopathic Principles and Practices in the ambulatory clinic setting, working one-on one with a preceptor where Osteopathic Manipulative Therapy (OMT) is delivered and performed.
In the inpatient setting on the family medicine teaching service, the residents round on patients who have been recognized as good candidates for OMT. While in this setting, they are observed, instructed, and evaluated by the attending physician staff on the OMT exam. The interns begin by observing upper year residents and faculty.
They also receive lectures and teaching on how to provide care incorporating the four tenets of Osteopathic Medicine - body unity, self-healing and self-regulatory mechanisms, and the interrelationship of structure and function.
As they progress, structured OMM clinics are built into their rotations. They are evaluated during these sessions and on their hospital rotations using checklists that assess their skills in provision of complete and accurate structural evaluation.
Osteopathic training is also achieved through assisting with MS3/MS4 OMT workshops at Philadelphia College of Osteopathic Medicine (PCOM) and partnering with them for ABOFP board preparation.


Residents have the opportunity to participate in immersive electives with the goal to learn more about global health, demonstrate cultural sensitivity as it relates to the location, and understand the cultural context of health and disease in resource-limited settings. Requested global health rotations are expected to be completed in a standard academic setting or with a global health provider/team.
The Northside Family Medicine residency program powers a Walk with a Doc chapter to promote physical activity. Learn More

An area of concentration is comprised of a predetermined group of electives within the scope of family medicine designed to focus on the resident’s future practice goals. Early in their training, residents have the opportunity to select or develop an individualized educational plan (IEP) to provide additional training above and beyond the core training in family medicine. In doing this, the needs of the resident’s future practice community are taken into consideration. Current offerings on a growing list of AOCs include Outpatient Medicine, Sports Medicine, Urgent Care, Rural, Maternity Care, and Hospice/Palliative Care.